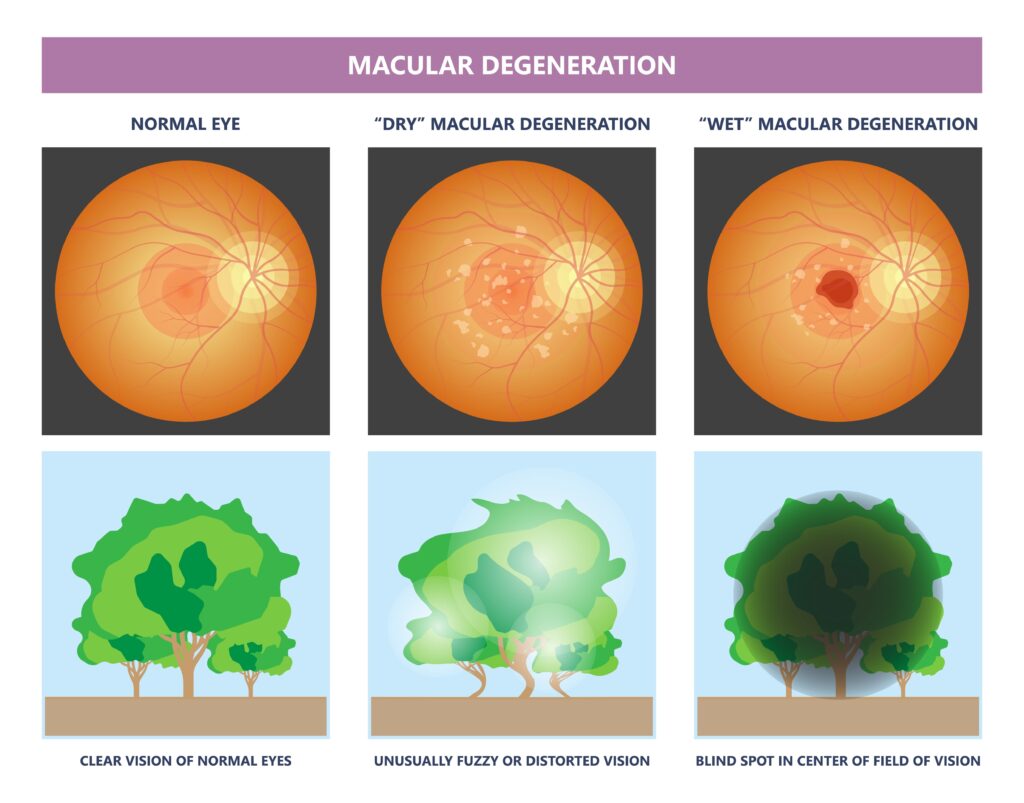
What is Macular Degeneration?
Macular degeneration is damage or breakdown of the macula of the eye. The macula is a small area at the back of the eye that allows us to see fine details clearly. When the macula doesn’t function correctly, we experience blurriness and darkness in the center of our vision. Macular degeneration affects both distance and close vision and can make some activities, like driving, threading a needle or reading, difficult or impossible.
Although macular degeneration reduces vision in the central part of the retina, it does not affect the eye’s side or peripheral vision. For example, you could see the outline of the clock but not be able to tell what time it is.
Recently it has become clear that genetics plays a major role in the susceptibility to macular degeneration and a positive family history in parents and siblings is a risk factor. Other risk factors include smoking, female gender and Caucasian race.
Macular degeneration is usually divided into two categories: wet and dry. The dry form is more common. In this case, the pigment layer behind the macula undergoes atrophy and can accumulate deposits of waste material, called “drusen”, which are visible to Dr. Greenberg as yellowish spots in the back of the eye.
Early on, dry macular degeneration may not affect the vision, but in more severe cases, vision can become blurred or blank areas may appear in the central vision. There is no known effective way of improving dry macular degeneration, but it has been proven that antioxidants Lutein and Zeathanthin, Zinc and vitamins E, and C, in specific doses, can slow progression and reduce the risk of vision loss.
What is Wet (exudative) Macular Degeneration?
Wet macular degeneration is the result of tiny abnormal new blood vessels that grow and break into the space behind the macula, causing leakage of blood and fluid. It is often preceded by dry degeneration. Dr. Greenberg can identify people who may be at risk for the development of this more severe form of the disease. Wet macular degeneration is less common, but when it occurs, can cause more serious loss of vision. Symptoms may begin as gradual progressive blurring or distortion of the vision. Straight objects such as telephone poles or venetian blinds may appear crooked. Sometimes the loss of vision occurs abruptly and with no warning.
What is Dry (atrophic) Macular Degeneration?
Dry macular degeneration has three stages: early, intermediate and late stage. Dry macular degeneration is progressive and can turn into wet macular degeneration if it is not diagnosed and treated in a timely manner. There is no known effective way of improving dry macular degeneration, but it has been proven that antioxidants Lutein and Zeaxanthin, Zinc and vitamins E, and C, in specific doses, can slow progression and reduce the risk of vision loss.
Macular degeneration can be diagnosed by Dr. Greenberg with a dilated fundus exam in the office. Many times other in-office testing, such as angiography, a photographic test involving the injection of intravenous dye, or ocular coherence tomography (OCT), a sophisticated digital imaging test of the macula, may be necessary to diagnose and formulate the appropriate treatment.
Frequently Asked Questions
Protect your vision – schedule an appointment today to manage macular degeneration with our expert care.

